The use of local cold therapy, also known as cryotherapy, has been a common practice in the management of acute musculoskeletal injuries such as strains, sprains and contusions for decades. Think of it as that bag of ice you put on your elbow after hitting two large buckets of range balls. Cold therapy is often lumped into the injury-treatment acronym “RICE”, as in, rest, ice, compression and elevation. The term was coined by Dr Gabe Mirkin in 1978 as treatment to enhance healing of minor injuries. But in 2019, Dr Mirkin wrote a mea culpa of sorts as a letter to the editor in the American Journal of Sports Medicine, essentially apologising en masse, stating newer research showed ice and rest might delay healing of minor injuries.
So should you be applying a frozen bag of peas to that sore knee or jump in an ice bath to recover after 36 holes? Or should you apply heat to sore areas to help recover faster? Here’s a review of what studies have concluded about the debate over ice vs heat.
Q: Which is more effective in injury treatment?
Research studies have shown that local application of cold can help in reducing the pain and swelling in acute musculoskeletal injuries. However, there is still some debate about whether cryotherapy can speed up the healing process or potentially slow it down.
One study published in the British Journal of Sports Medicine analysed data from 34 clinical trials on the effects of cryotherapy on musculoskeletal injuries. The study found that while icing provided short-term pain relief and reduced swelling, there was no clear evidence to support its use in accelerating the healing process or improving functional outcomes. Overall, the evidence suggests that while cryotherapy can provide short-term benefits in managing acute musculoskeletal injuries, it might not necessarily speed up the healing process. Ice application is more beneficial in pain reduction in the acute phase of joint injuries than heat, but other factors such as active rest, rehabilitation exercises, and proper medical care might play a more significant role in promoting healing.
Heat application, meanwhile, when combined with stretching can be more effective for delayed muscle pain and stiffness from exercising too strenuously. However, excessive or prolonged heat application can have detrimental effects on the healing process. For example, heat can increase inflammation and swelling in the injured area if applied during the first five to seven days after injury or re-injury (from a return to the golf course too soon, for instance). That means you’re possibly delaying recovery and making pain and stiffness worse. Heat can also increase metabolic demand in the tissues, which can lead to increased tissue breakdown and delayed repair. Also, heat applied later in recovery or to old injuries can aid in range of motion improvement and tissue extensibility, and could be helpful at improving movement in body parts challenged by a chronic injury before golf or other activities.
Overall, the evidence suggests that local heat application can be beneficial when used about a week after an injury occurs. A general rule: use ICE (ice, compression, elevation) in the first 48 hours to control pain, but after that, it might be better to use compression, elevation and controlled movement for swelling. (NOTE: these guidelines are suggested for acute athletic injuries and not post-surgical cases).
Q. I’m not hurt. I’m just sore from exercise. Should I use ice or heat?
Delayed onset muscle soreness (known as “DOMS”) occurs after hard or unaccustomed load to your muscles through exercise or sport. It usually peaks 48 hours after your activity and can be incredibly limiting in terms of range of motion and pain. Neither heat nor ice is better than the other at relieving DOMS pain, but there is some indication that ice might delay muscle regeneration. Therefore, it’s best to apply 15 to 20 minutes of heat with some gentle stretching.
Q. What about alternating between hot and cold treatments?
Known as contrast therapy, immersing a part of the body in alternating treatments of hot and cold water, has been shown to be more effective than doing nothing for swelling reduction, but not more effective in treatment than using just ice.
Contrast therapy has become very popular and if you do try it, it’s best if you finish the alternating treatments with cold. Typical applications are 10 to 15 minutes of heat followed by 10 to 15 of cold, up to an hour total.
Q. What’s the best way to use ice?
Keep a barrier between the ice and your skin to avoid burns and, albeit rare, damage to nerves close to the skin’s surface. For example the nerve that travels behind the top of the small bone of the lower leg (fibula) at the outside of the knee can be damaged by direct application of ice.
Also, don’t use ice for more than 20 minutes at a time. An intermittent approach of 10 minutes ice followed by 10 minutes of room-temperature recovery over a two-hour period during the first week after injury might be the most effective.
Q. Is there a danger that using ice will hurt my performance on the golf course?
Published evidence, as well as clinical experience, show power development and balance to be unaffected at the joints, such as the ankles and knees. However, icing areas with more muscle, such as the shoulders and thighs, can impede movement until those tissues have warmed again.
Q. I have arthritis. Does ice or heat help with the pain?
Arthritic inflammation is not that same as a minor acute or athletic injury, and ice can be very effective at reducing arthritic joint pain after activity. Heat applied to non-swollen arthritic joints before activity might improve mobility and pain prior to golf, but it varies from person to person.
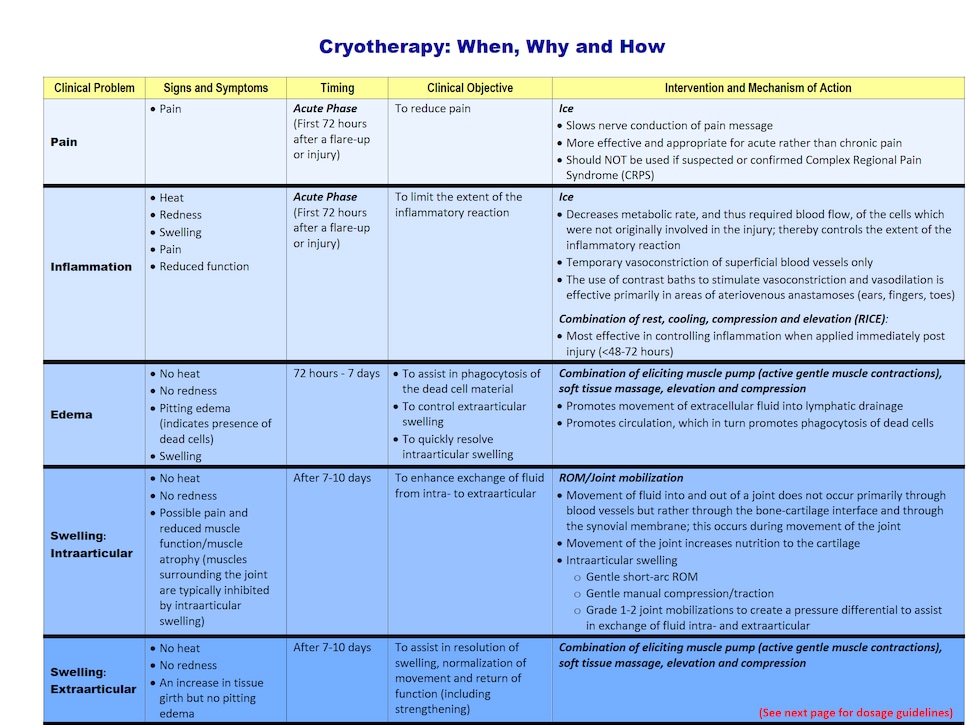

Here is a really useful chart from the University of British Columbia’s department of physical therapy.
Golf Digest Professional Adviser Ralph Simpson was a physical therapist on the PGA Tour for 11 years and owns Manual Orthopedic and Sports Therapy in Whitefish, Montana.



